Can diabetes cause problems in your feet-skin?
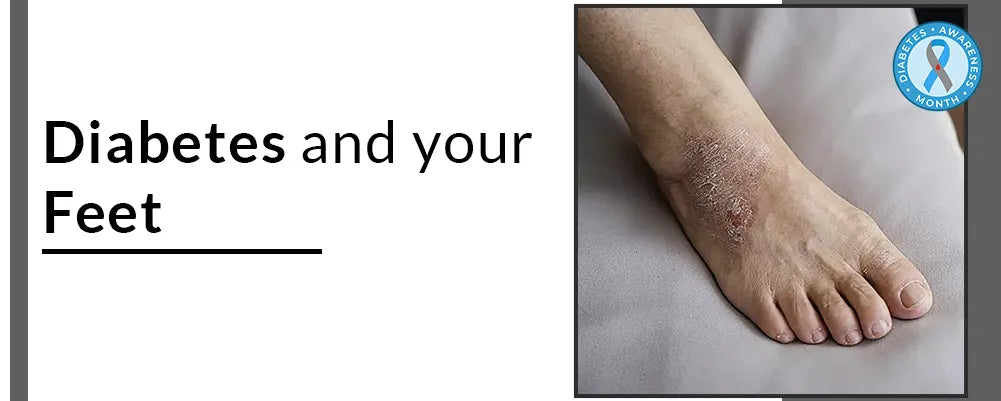
Living with diabetes involves a series of challenges, and one aspect that often goes overlooked is foot health. Diabetes can have a deep effect on various parts of the body, and the feet are no exception. Complications arising from diabetes can lead to serious problems with the skin on your feet. In this blog post, we will explore, connection between diabetes and foot skin issues and how you can maintain happy and healthy feet.
The Diabetes-Foot Skin Connection: Diabetes is known to affect blood circulation and nerve function, and the feet are particularly vulnerable to these changes. High blood sugar levels can damage nerves (neuropathy) and reduce blood flow (peripheral arterial disease). These complications make the feet vulnerable to infections, slow healing, and skin issues.

- Dry Skin: One of the common problems individuals with diabetes face is dry skin on their feet. Neuropathy can cause decreased sweating, leading to dryness. Cracked and dry skin becomes more prone to infections, posing a risk for individuals with diabetes.
- Fungal Infections: Diabetes can make it easier for fungi to grow.6. Athlete's foot and toenail fungus are prevalent among individuals with diabetes due to compromised immunity and poor blood circulation.
- Ulcers and Wounds: Neuropathy can cause a loss of sensation in the feet, making it challenging to detect injuries. Combined with poor blood circulation, even minor wounds or ulcers may take longer to heal, increasing the risk of infection.

Tips for Diabetic Foot Care:
Alongside using specialised foot creams, Individuals with diabetes should adopt a comprehensive approach to foot care which includes
- Daily Inspection: Regularly inspect your feet for any cuts, blisters, or sores. Early detection is important in preventing complications.

- Use of Foot Creams: Diabetes can lead to dry skin, and the feet are particularly susceptible to many skin problems. Foot creams provide moisturization, prevent fungal infections, callus & corn, support wound healing, improve circulation and prevent complications like foot ulcers and infections.
- Proper Footwear: Choose comfortable shoes that provide adequate support. Avoid tight or ill-fitting shoes that can cause friction and pressure points.
- Regular Exercise: Physical activity improves blood circulation. Incorporate regular exercise into your routine, as advised by your healthcare provider.
- Control Blood Sugar Levels: Keeping blood sugar levels within the target range is vital for overall health, including foot health.

Diabetes demands a holistic approach to healthcare, and foot health should not be overlooked. A Foot Cream, with targeted formulation, can be a valuable addition to your diabetes management routine. Remember, maintaining healthy feet is a proactive effort that involves a combination of proper skincare, regular monitoring, and adherence to medical advice. Taking care of your feet today can prevent complications tomorrow, allowing you to stride confidently on your journey with diabetes.








